Smile Visualization
Take a smiling selfie and we’ll show you what Invisalign® treatment can do for you. Sometimes insurances can cover upto $2500 of invisalign treatment. Call our office or follow the link to find out.
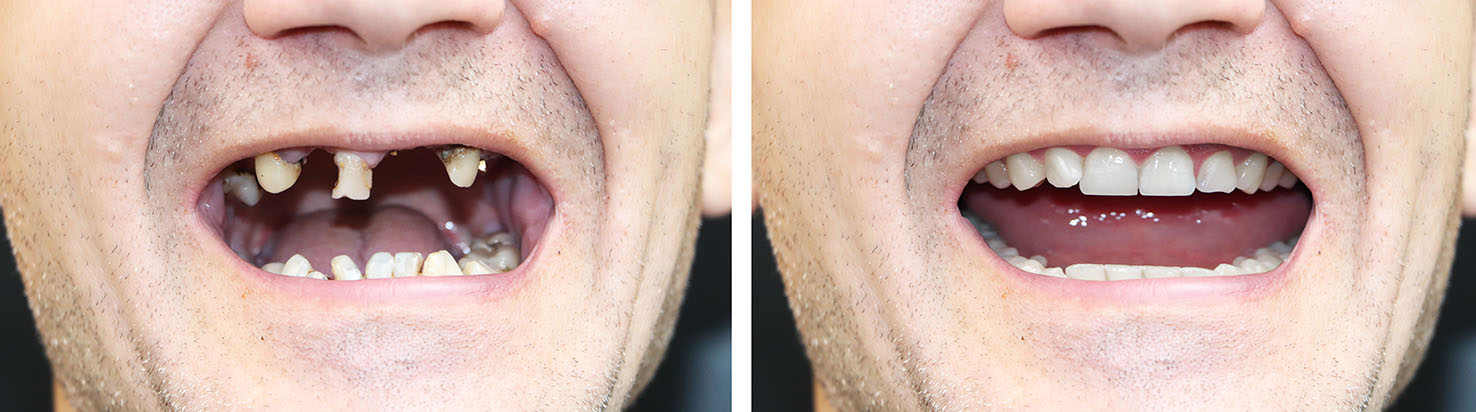
Missing teeth affect far more than appearance — they influence how you eat, speak, and how your jaw and facial tissues hold up over time. Many adults experience tooth loss from decay, gum disease, or injury, and modern implant dentistry offers a durable, biologically sound option to restore both function and confidence. Rather than simply covering a gap, implants are designed to replace the tooth root and support a lifelike replacement tooth.
The goal of implant treatment is to recreate the stability and comfort of a natural tooth so patients can chew freely, speak clearly, and smile without worry. Advances in implant materials, imaging, and surgical techniques make it possible to deliver predictable, long-term outcomes that integrate with a patient’s unique oral anatomy. Careful planning and precise placement are central to success.

Unlike removable prosthetics that sit on top of the gums, dental implants are surgically anchored into the jawbone where they act much like natural tooth roots. This anchorage stabilizes crowns, bridges, or dentures and restores a bite that feels familiar. The result is a restoration that looks, feels, and performs more like a natural tooth than traditional alternatives.
Because implants transmit biting forces to the underlying bone, they help maintain bone volume and facial contours — an important benefit for preserving long-term oral health and aesthetics. When planned and executed correctly, an implant-supported restoration can remain a dependable part of the mouth for many years with routine care.
Dental implants are typically made from biocompatible materials that encourage the surrounding bone to grow and bond to the implant surface, a process called osseointegration. This biological fusion is what gives an implant its unique strength and stability. The timeline for integration varies, but once complete, the implant becomes a fixed base for a prosthetic tooth.
Modern implant planning often uses 3D imaging and digital impressions to map the jaw and identify the optimal implant position. This level of precision reduces surprises in surgery and helps the restorative team design a final crown or bridge that fits comfortably and looks natural. Patients are guided through each stage so they understand the sequence and expected healing milestones.
Beyond improved chewing and speech, implants offer a series of practical benefits that affect daily life. They eliminate the slipping or shifting associated with many removable dentures, reduce the need to modify adjacent healthy teeth, and restore the confidence to enjoy all types of food without restriction. Implants are also resistant to decay, which changes the maintenance focus toward gum health and prosthetic care.
When supported by a clear maintenance plan — regular cleanings, home hygiene, and periodic professional evaluations — implant restorations provide a long-term solution that supports both oral health and overall quality of life. The clinical benefits combine with the cosmetic improvements to deliver results patients can rely on.
For patients exploring options, a consultation at Fuller Smiles San Fernando Valley provides a thorough review of candidacy, treatment alternatives, and the practical implications of choosing implants as a restorative solution.
Candidacy for implants is based on factors such as overall health, oral hygiene, jawbone volume, and personal goals for comfort and appearance. Many people who are otherwise healthy are good candidates, but conditions that affect healing — like uncontrolled systemic disease or certain medications — require careful evaluation. A comprehensive exam and imaging help determine whether implants are appropriate.
When bone volume is limited, adjunctive therapies like bone grafting or sinus elevation can create a stable foundation for implants. These preparatory steps are common and are discussed openly as part of a patient-specific treatment plan that balances risk, timeline, and long-term prognosis.
Implant therapy begins with a diagnostic phase: clinical examination, digital imaging, and the development of a restorative plan. Surgical placement of the implant is typically performed in an outpatient setting and is often well tolerated with local anesthesia and optional sedation. The number and complexity of implants determine the length and steps of the procedure.
After implantation, a healing period allows osseointegration to occur. Temporary prostheses can often be provided so patients have function and aesthetics while the final restoration is being fabricated. Once integration is confirmed, a laboratory-crafted crown, bridge, or denture is attached to the implant to complete the restoration.
Bone grafting is a predictable method to rebuild lost jawbone and create a secure site for implant placement. Bone loss can result from long-standing tooth absence, periodontal disease, or trauma. By augmenting the deficient area with graft material, clinicians restore volume and contour so an implant can be placed in an ideal position.
The decision to graft is individualized: some cases allow for simultaneous grafting and implant placement, while others require staged treatment where grafting occurs first and an implant is placed after healing. The choice depends on the quality and quantity of existing bone and the overall treatment objectives.
Beyond grafting, additional measures like soft tissue management, sinus lifts, and periodontal therapy can improve the predictability and longevity of an implant restoration. Addressing gum health before or during implant therapy reduces the risk of complications and helps ensure that implants function harmoniously with the surrounding tissues for years to come.
Clear communication between surgical and restorative clinicians — plus patient engagement in oral hygiene — is essential. When everyone shares the same priorities, the result is a stable, natural-looking restoration that fits the patient’s lifestyle and oral health goals.
Implant dentistry is as much about long-term planning as it is about immediate results. By combining modern imaging, prosthetic design, and surgical precision, clinicians create solutions that balance function, comfort, and appearance. Patients who invest in this level of care benefit from restorations that perform well and require routine maintenance similar to natural teeth.
At Fuller Smiles San Fernando Valley, our approach emphasizes careful assessment, individualized treatment sequencing, and clear patient education so you can make an informed decision about implant care. If you’re considering tooth replacement, learning how implants may fit into your oral health plan is the first step toward a durable and natural-feeling solution.
Dental implants offer a versatile and reliable pathway to restore missing teeth, protect jawbone health, and regain everyday comfort with eating and speaking. Whether you need a single tooth replaced or a full-arch solution, modern implant workflows provide predictable results when planning and execution are prioritized.
If you’d like to explore implant options further or have questions about the process, please contact us for more information and to arrange a consultation. Our team is ready to discuss your needs and help you determine the best path forward for rebuilding a confident, healthy smile.
If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are small, biocompatible posts that are surgically placed into the jawbone to replace missing tooth roots. Most implants are made from titanium or titanium alloy, materials that are well tolerated by the body. Once positioned, the implant provides a stable foundation for a crown, bridge, or denture.
Over several months the implant fuses with the surrounding bone through a process called osseointegration, creating long-term support. After integration, an abutment is attached to the implant and a custom dental prosthesis is secured to restore function and appearance. This combination of implant and restoration closely mimics the look, feel, and chewing performance of natural teeth.
Good candidates for dental implants are generally healthy adults who are missing one or more teeth and have sufficient jawbone to support an implant. Controlled chronic conditions such as well-managed diabetes or stable heart disease do not automatically rule out implants, but they require careful evaluation. Smoking, untreated periodontal disease, and certain medications can affect healing and the likelihood of long-term success and should be discussed with your dentist.
At Fuller Smiles San Fernando Valley each potential implant patient receives a comprehensive assessment including clinical examination and radiographic imaging to evaluate bone volume, nerve proximity, and sinus anatomy. If bone or soft-tissue limitations exist, the treatment plan may include grafting or staged procedures to create a stable foundation for implants. Your dentist will explain alternatives and tailor a plan that matches your oral health, cosmetic goals, and overall medical profile.
Dental implant restorations range from single-tooth crowns to implant-supported bridges and removable or fixed full-arch solutions. A single implant and crown replace one missing tooth without altering neighboring teeth, while implant-supported bridges replace multiple adjacent teeth using strategically placed implants. Full-arch options such as an implant-retained denture or a fixed prosthesis supported by four to six implants can restore an entire jaw.
Removable implant-retained overdentures attach to locator or bar systems, offering improved retention compared with conventional dentures. Restorations are custom fabricated from materials chosen for strength and esthetics, including ceramic crowns and hybrid prostheses for full-arch cases. Selection of the appropriate restoration depends on your functional needs, bone anatomy, and long-term maintenance considerations.
The implant placement process begins with detailed planning that typically includes a clinical exam, digital imaging such as CBCT, and development of a surgical guide when needed. On the day of surgery the implant is placed under local anesthesia, often with the option of oral or IV sedation for patient comfort. The surgical procedure itself is usually performed on an outpatient basis and can vary in length depending on the number of implants and any concurrent procedures.
After placement the implant is allowed to heal and integrate with the bone; this healing phase is monitored through follow-up visits and imaging. Once adequate integration is achieved, an abutment is connected and impressions are taken to fabricate the final prosthesis, which is then adjusted for fit and bite. Your dental team will provide detailed preoperative and postoperative instructions to support healing and minimize complications.
Bone grafting is recommended when the jaw lacks sufficient height or width to support a dental implant safely and predictably. Bone can be lost following tooth extraction, chronic infection, or long-term denture wear, and grafting rebuilds the volume needed for secure implant placement. Grafts may use the patient's own bone, donor bone, or synthetic grafting materials depending on the clinical situation and the dentist's recommendation.
The goal of grafting is to provide a stable environment for osseointegration and to optimize long-term implant success. Timing for grafting varies: some patients receive grafts at the time of tooth extraction, others have grafting as a separate preparatory procedure before implant placement. Healing after grafting can take several months, and the treatment timeline is determined by the extent of augmentation and individual healing response.
Healing and integration of a dental implant typically take several months and depend on factors such as implant location, bone quality, and any adjunctive procedures like grafting. In general, implants placed in the lower jaw may integrate faster than those in the upper jaw due to denser bone, and grafted sites may require additional healing time. Clinicians commonly plan a healing interval of three to six months before loading an implant with a final restoration to ensure stable osseointegration.
Some treatment protocols allow for immediate placement of a temporary crown or bridge on the same day as surgery, but these provisional restorations are used selectively based on primary stability and case complexity. Final prostheses are delivered once integration is confirmed, and the restorative team adjusts fit, occlusion, and esthetics during try-in appointments. Your dentist will explain expected timelines specific to your case and provide guidance for care during each healing phase.
Dental implants offer superior stability and function compared with removable dentures and avoid the need to alter adjacent healthy teeth as with traditional bridges. Because implants stimulate the underlying bone, they help preserve jawbone volume and maintain facial contours that might otherwise diminish after tooth loss. Implants are made from materials that do not decay and provide a predictable foundation for chewing, speaking, and smiling with confidence.
Implant restorations are designed to be durable with routine care and regular professional maintenance, reducing the likelihood of frequent prosthetic replacements. In many cases implants allow patients to eat a wider variety of foods and experience fewer dietary restrictions than with conventional removable prostheses. Your dental team will review the long-term care plan to help you maximize the longevity and performance of your implants.
Caring for dental implants requires the same diligent oral hygiene practices recommended for natural teeth, including twice-daily brushing and daily interdental cleaning. Interdental brushes, floss designed for implants, and low-abrasive toothpaste can help remove plaque around implant components without damaging prosthetic materials. Professional dental cleanings and periodic examinations are essential to monitor tissue health, check attachment components, and address early signs of inflammation.
Avoiding tobacco and minimizing habits that place excessive force on teeth, such as hard chewing or nail-biting, further protects implant longevity. If you have an implant-retained overdenture or specialized prosthesis, your dental team will instruct you on removal, cleaning, and reattachment procedures specific to that design. Communicate any looseness, discomfort, or changes in bite to your dentist promptly to allow early evaluation and treatment.
As with any surgical procedure, dental implant treatment carries potential risks, including infection, bleeding, or delayed healing in some patients. Other complications can include nerve irritation or injury, sinus involvement for upper jaw implants, and failure of the implant to integrate with the bone. While the overall success rate for implants is high, these complications can occur and usually require prompt assessment and management.
Certain factors such as uncontrolled systemic disease, smoking, poor oral hygiene, or inadequate bone can increase the likelihood of complications and are addressed during the treatment planning process. If a problem arises, treatment options range from conservative management with antibiotics and local care to surgical intervention or replacement of the implant in select cases. Your dentist will explain potential complications relevant to your situation and outline how they are prevented and treated.
The office of Fuller Smiles San Fernando Valley prepares patients through careful diagnostics, clear communication, and a tailored treatment plan that addresses medical history, imaging findings, and aesthetic goals. Preoperative instructions cover oral hygiene, medication management, and expectations for anesthesia or sedation to ensure a safe and comfortable experience. The team coordinates any necessary referrals, laboratory work, or grafting procedures and schedules follow-up visits to monitor healing and prosthetic integration.
Patient education includes step-by-step explanations of the surgical and restorative phases so individuals understand what to expect at each stage. On the day of surgery the clinical team prioritizes comfort, sterile technique, and precise implant placement guided by preplanned digital or analog guides. Aftercare instructions and emergency contact information are provided to support recovery, and the practice schedules restorative appointments to finish the final prosthesis once healing is complete.

Take a smiling selfie and we’ll show you what Invisalign® treatment can do for you. Sometimes insurances can cover upto $2500 of invisalign treatment. Call our office or follow the link to find out.